Staying informed is an important part of protecting people, workplaces, and communities. In response to recent questions around Hantavirus, we have gathered clear, information and practical resources to help our customers and partners understand the topic and know where to find reliable guidance.
What you need to know
Hantavirus is a known virus that public health authorities continue to monitor. While cases remain limited, access to accurate information is key to avoiding misinformation and unnecessary concern. Our goal is to share science‑based insights and explain what this means in practical terms for businesses and facilities.
Origins
Hantaviruses are members of the Bunyaviridae family of viruses. The virus is commonly found in rodent populations, such as rats and mice, and can spread to people from contact with the rodents, their urine, feces, and saliva, and their bedding. Bites or scratches from infected rodents can transmit the virus, but this is relatively rare. These viruses can cause severe illness and death from diseases such as Hantavirus Pulmonary Syndrome (HPS) and Hemorrhagic Fever with Renal Syndrome (HFRS). Hantavirus Infections are particularly dangerous because they impede lung function.
Geographic Risk of Exposure and Source/Natural Reservoir
People can become infected with Hantaviruses anywhere in the world where rodents are present. HPS is primarily found in the Western Hemisphere, while HFRS is mostly found in Europe and Asia. There are exceptions as Seoul virus, which is a type of Hantavirus that causes HFRS, can be found worldwide.
Rodents pass Hantaviruses within their populations. Once infected, a rodent can secrete the virus in its urine, saliva, and feces for a long period of time and potentially for the rest of its life. The rodents are not believed to show symptoms of being infected, so it is not likely that they can be identified visually from other uninfected rodents. There are a range of Hantaviruses that can cause Hantavirus infection in people. Each Hantavirus is typically associated with a specific rodent species as its primary reservoir.
Symptoms
HPS symptoms typically occur 1-8 weeks exposure. Early symptoms include:
- Fatigue
- Fever
- Muscle aches, especially in large muscle groups
Some people with HPS also experience:
- Headache
- Dizziness
- Chills
- Abdominal issues, such as nausea, vomiting, diarrhea, and abdominal pain
For some people, their infection does not progress past the initial symptoms. For others, the disease progresses, and additional symptoms appear. From 4 to 10 days after the initial symptoms, additional symptoms can appear, such as:
- Coughing
- Shortness of breath
- Tightness in the chest
When people with HPS develop respiratory symptoms, there is a 38% mortality rate, though this number has reached 50% in some reports.
HFRS symptoms typically develop within 1-2 weeks after exposure but can take up to 8 weeks in some cases. Initial symptoms include:
- Intense headaches
- Back and abdominal pain
- Fever/chills
- Nausea
- Blurred vision
Some people may develop flushing of the face, inflammation or redness of the eyes, or a rash. Later symptoms indicating a more serious form of the disease can include:
- Low blood pressure
- Shock/lack of blood flow
- Internal bleeding
- Acute kidney failure
HFRS is fatal in 1-15% of cases. Complete recovery can take up to several months.
Method of Transmission/Contagiousness
Hantavirus infection is a zoonotic disease, meaning most people become infected from exposure to infected rodents. The urine, saliva, and feces of rodents can be contaminated with Hantavirus, and when the urine or feces are ingested or inhaled, people can be exposed to the virus and become infected. Touching contaminated objects, eating contaminated food, exposure to open cuts or sores on a person’s skin, and being bitten or scratched by an infected rodent can also cause infection. Inhalation of dried urine, saliva, or feces containing the virus, such as through cleaning, can also cause transmission. People with cuts in their skin are more susceptible to being infected by contaminated urine, saliva, feces, or nesting materials, especially when not wearing gloves during cleaning.
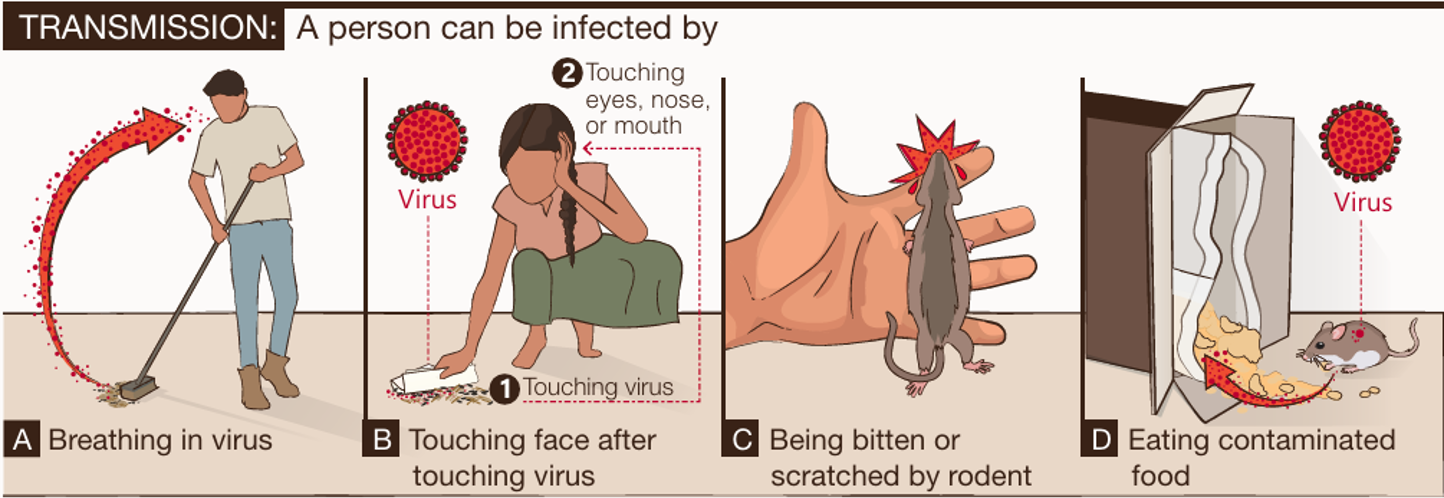
Figure 1 - How do people get HPS. Source: U.S. Centers for Disease Control and Prevention
Hantavirus is generally not transmitted from person to person, and casual contact, such as skin-to-skin contact without body fluid exchange is not believed to be capable of transmitting Hantavirus. It is unclear whether a person needs to be symptomatic to transmit Hantavirus virus to other people. The exception is the Andes strain which appears to be more readily transmissible between people via respiratory secretions or bodily fluids.
Transmission of Hantavirus is generally more common in rural areas likely to have larger rodent populations but can occur in urban areas as well. Dogs and cats are not known to become infected with Hantavirus but may bring infected rodents into homes, creating a risk of transmission. Dead rodents should always be handled with caution.
Prevention and Risk Reduction
Vector/Pest Control – Since most cases of Hantavirus Infection are associated with exposure to infected rodents, the primary method of prevention is an effective pest control program to eliminate rodents and their bedding/nesting areas and education programs for the public about how to reduce rodent populations. Control of trash and food to avoid attracting rodents is helpful in preventing their presence. Ensuring buildings are sealed and do not offer entrance to rodents is also important. Any openings in a building should be sealed and rodent traps should be used when rodent infestation has occurred. Cleaning rodent droppings, dried urine or saliva, and bedding can disseminate the virus onto people or in the air, where it can be inhaled or swallowed. Inhalation of the virus that has become airborne is believed to be the most common method of exposure for people.
Reduce Contact – Uninfected people should avoid or minimize contact with people who have a Hantavirus infection until they have been treated by a doctor, even though the risk of person-to-person contact is minimal. If around an infected person, avoid coming in contact with blood, body fluids, or respiratory secretions and perform hand hygiene promptly if exposure occurs.
Vaccinations – There is currently no vaccine to prevent a Hantavirus Infection. Most people who develop Hantavirus infections eventually recover. It is unknown whether recovery from Hantavirus infection grants immunity from further Hantavirus infections.
Surface Cleaning/Disinfection – Hantaviruses are large, enveloped single-strand RNA spherical viruses that are members of the Bunyaviridae family of viruses and are easy to inactivate using chemical disinfectants. Since Hantavirus is commonly spread through exposure to infected rodents, their urine, saliva, and feces, and their bedding, frequent surface cleaning and disinfection of surfaces that may have been in contact with rodents is considered a primary method to reduce the risk of infection. People performing cleaning and disinfection activities where there are rodents or their droppings should wear appropriate personal protective equipment (PPE) to prevent exposure. At a minimum, people should wear gloves during cleaning and wash their hands thoroughly after removing gloves. Because inhalation of the virus from dried urine or saliva or droppings commonly occurs, additional PPE (gown, mask, goggles or face shield) is prudent when cleaning up an infestation and to avoid dry cleaning methods, such as dry dusting, sweeping, or vacuuming. Wet/damp cleaning methods are preferred to reduce the likelihood of viral dissemination into the air.
Hand Hygiene – Since Hantavirus is primarily spread through exposure to rodent urine, saliva, or feces, frequent hand hygiene with soap and water or the use of alcohol-based hand rubs reduces the risk of infection through environmental transmission.
Transmission-Based Precautions – For a suspected case of Hantavirus infection, standard precautions are recommended by the CDC and WHO. If the patient has Andes virus, the patient should be placed on airborne isolation. The use of gloves, fluid resistant gowns, eye protection, and respirator are recommended for direct patient contact.
Isolation – Patients suspected of having Hantavirus infection should be isolated from other patients in healthcare facilities to prevent exposure to other patients.
Fabric Handling – Ensure soiled fabrics from Hantavirus infection patients are handed in a way to prevent transmission (i.e. minimize agitation), using standard precautions. Healthcare laundering procedures for contaminated fabric are capable of making the fabric hygienic. Soiled laundry (e.g., bedding, towels, personal clothing) should be handled in accordance with recommended standard healthcare practices, which include prompt containment in an appropriate laundry bag and avoidance of shaking or agitating in manner that may disperse infectious material.
Good Health Practices - Practicing good health is also helpful in preventing the development of many illnesses. The strength of a person’s immune system is often related to their overall health. Getting plenty of sleep, eating healthy, avoiding smoking or being around cigarette smoke, being physically active, managing stress, maintaining an appropriate weight, and drinking plenty of water or other fluids can help keep your immune system strong.
Download our Hantavirus: Essential Information whitepaper for a complete overview you can easily reference and share
References and Useful Websites
Reference materials on Hantavirus Infections are available from the Centers for Disease Control and Prevention (CDC) and World Health Organization (WHO) websites. Many of these resources were used as references for the creation of this content.
- https://www.cdc.gov/hantavirus/about/index.html
- https://www.cdc.gov/hantavirus/hcp/clinical-overview/hps.html
- https://www.who.int/news-room/fact-sheets/detail/hantavirus